Using the PDCA Cycle for Continuous Improvement in Healthcare
Introduction
Continuous improvement is essential for healthcare organizations striving to enhance quality, safety, and operational efficiency. One of the most widely used methodologies for structured improvement is the PDCA Cycle, also known as the Plan–Do–Check–Act cycle.
Originally developed for quality management in industry, the PDCA framework has become a powerful tool for healthcare organizations seeking systematic and sustainable improvement.
By following a structured cycle of planning, testing, evaluating, and refining processes, healthcare teams can identify problems, implement solutions, and continuously improve patient care outcomes.
What is the PDCA Cycle?
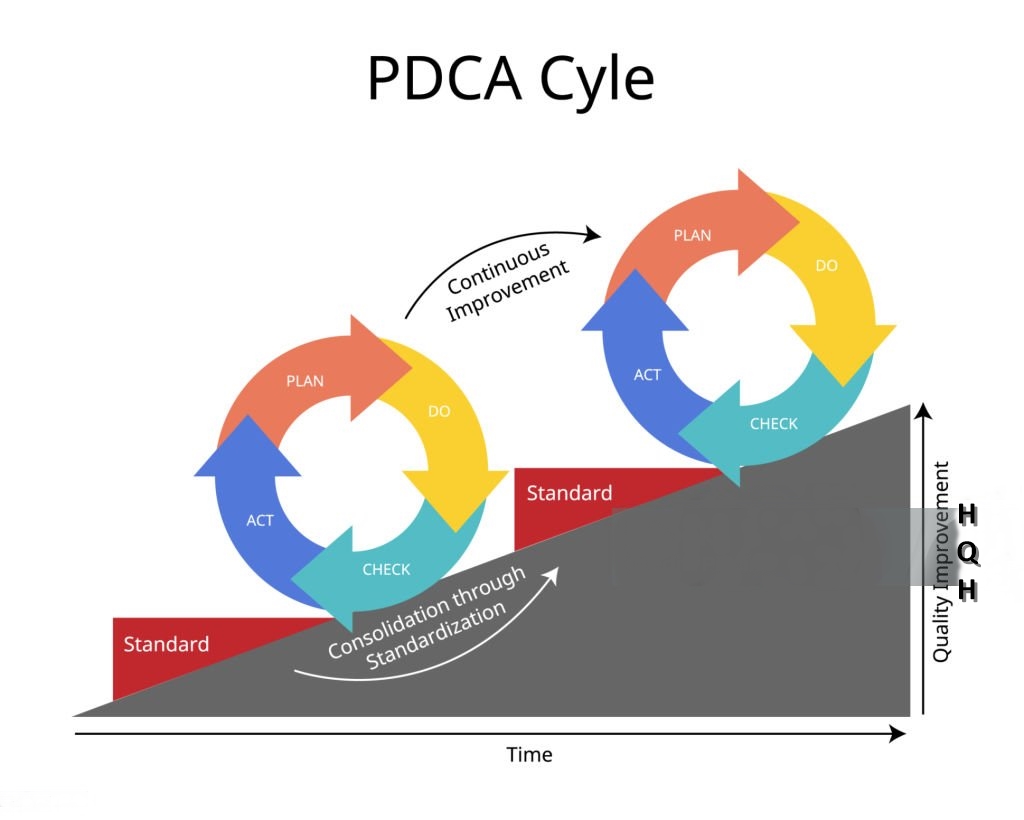
The PDCA Cycle is a four-step iterative method used for improving processes and solving problems.
The cycle consists of:
-
Plan – Identify a problem and design a solution
-
Do – Implement the solution on a small scale
-
Check – Evaluate the results and measure performance
-
Act – Standardize the improvement or refine the approach
This structured method allows organizations to test improvements while minimizing risk.
Step 1: Plan
In the planning phase, healthcare teams identify a problem or improvement opportunity.
This stage typically involves:
-
Analyzing current processes
-
Identifying root causes of problems
-
Defining measurable objectives
-
Developing an improvement plan
Data collection and stakeholder involvement are essential during this phase.
Step 2: Do
During the “Do” phase, the proposed solution is implemented on a small scale or pilot basis.
This approach allows healthcare teams to test whether the proposed change produces the desired improvement without disrupting the entire system.
Proper documentation of activities and outcomes is important for later evaluation.
Step 3: Check
In the evaluation phase, teams review the results of the implemented change.
This involves:
-
Measuring performance indicators
-
Comparing results with expected outcomes
-
Identifying any unintended consequences
The goal is to determine whether the change has effectively addressed the original problem.
Step 4: Act
In the final phase, organizations decide how to proceed based on the results.
Possible actions include:
-
Standardizing the successful improvement across the organization
-
Adjusting the strategy and repeating the cycle
-
Identifying additional opportunities for improvement
The PDCA cycle then repeats, creating a culture of ongoing improvement.
Benefits of Using PDCA in Healthcare
Healthcare organizations that implement PDCA effectively can experience several benefits:
-
Improved patient safety and care quality
-
Better teamwork and communication
-
Data-driven decision-making
-
Reduced operational inefficiencies
-
Stronger culture of continuous improvement
Because the method is simple yet structured, it can be applied across clinical, administrative, and operational processes.
Conclusion
The PDCA Cycle provides healthcare organizations with a practical and structured approach to continuous improvement. By systematically planning, testing, evaluating, and refining processes, healthcare teams can address challenges effectively and achieve sustainable improvements in quality and safety.
Organizations that embed PDCA into their quality management systems are better positioned to adapt, innovate, and deliver higher standards of patient care.